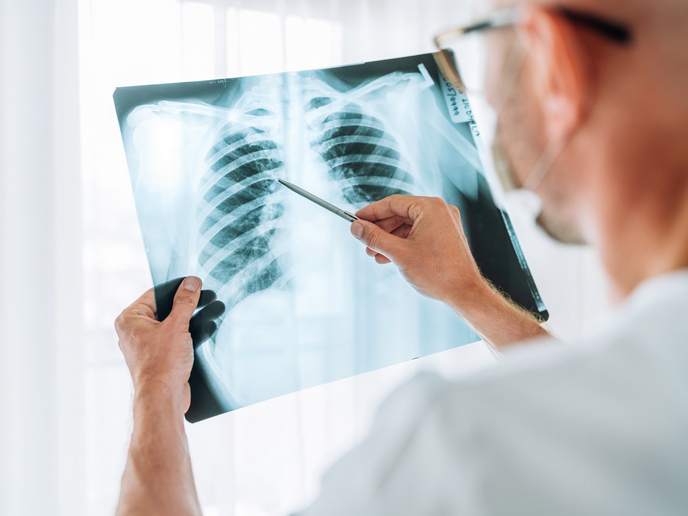
Boosting lung function in cured TB patients
Tuberculosis (TB) has historically been the most common infectious cause of death globally. Although it is preventable and curable, continued unequal access to medication, along with environmental factors often linked to poverty, have seen the disease persist into the 21st century. “The disease is also constantly evolving,” says DRTB-HDT(opens in new window) project manager Anne Jacobs from the Swiss Tropical and Public Health Institute(opens in new window). “As a result, we are seeing increasing levels of drug-resistant TB, along with less effective medication.” Indeed, cases of the drug-resistant (rifampicin-resistant (RIF-R)) form of TB have magnified the global health threat of the disease.
New strategies to improve lung function
In addition to these well-recognised shortcomings, current TB treatments – particularly those for RIF-R TB – often leave cured patients with serious lung impairments. This can shorten their lives and leave them with lifelong disability. This is what the EU-funded DRTB-HDT project sought to address. More specifically, the project wanted to see if new host-directed therapies (HDTs) could improve the recovery of lung function in TB patients. HDTs aim to treat infections and diseases by targeting a patient’s own biological pathways, rather than attacking the pathogen itself. For this, two existing medications were identified and repurposed – C-11050 and metformin. These drug candidates were selected to reduce inflammation and induce host cell antimicrobial activity, respectively. “We were really focusing on what happens after a patient has been treated for TB,” explains Jacobs. “Can we help their lungs to recover better by giving their immune system a boost?”
Randomised global trials and population modelling
At the heart of the project was a randomised global trial. Some 330 patients were selected from Georgia, Moldova, Mozambique, Romania and South Africa. The idea was to understand the situation in regions where TB is declining, such as Europe, as well as in regions where TB continues to pose a more widespread threat, such as southern Africa. “There were initially a number of challenges to overcome, such as sourcing the drugs and dealing with the COVID pandemic,” adds Jacobs. “When we started the trial, many TB patients also suffered from the impacts of the COVID pandemic.” Once the trial was up and running, all patients received a standard multidrug TB therapy, and in the experimental trials additionally received either CC-11050 or metformin. Patients blew into a spirometer, which measured how much air they could expel, to help gauge improvements in lung function. The project also carried out modelling work to assess the potential impact a successful HDT might have on individual health and population resilience.
Potential for successful HDT interventions
While the spirometer tests did not reveal the significant improvements in lung function that were hoped for, many positive clinical lessons were learned. Clinicians for example noted that spirometry takes practice to do properly and can sometimes be uncomfortable for patients. This feedback will help us learn how to do this better in future studies. The modelling work also demonstrated that a successful HDT intervention would likely bring huge health and economic benefits for both individuals and societies as a whole. “We showed that improved lung function would be a great investment for healthcare systems,” notes Jacobs. “Patients would be more able to return to work and live more healthy years.” The DRTB-HDT team is looking to continue this avenue of research through sharing findings with projects funded under the same programme(opens in new window). “Knowing what HDT procedures work and what don’t will help us to focus on moving forward,” she says.